“In BC in 2015, 828 babies were born to mothers under age 20.[9] There are social, educational, and physical risks associated with unintended pregnancy in adolescence.[10] Unintended teen pregnancies are associated with poorer educational achievement and lower income for the mother. Babies born to teen mothers are more likely to be born preterm and small for gestational age, which increases the risk for a stay in a neonatal intensive care unit.[11]
At sexual health clinics across the province, oral contraceptives are often the only contraception choice available for free, despite evidence that LARC is more effective and cost-efficient.[12] While it is laudable that a hormonal IUD is on the Fair Pharmacare formulary, there remain potential barriers for teens whose families may qualify for Fair Pharmacare—the family may not be signed up, or they may not have met their annual deductible yet. For teens from families who do not qualify for Fair Pharmacare, the burden is on the teen to either buy the IUD or ask for financial assistance from their family. Because confidentiality is a foundational aspect of adolescent care,[13] and sexual health care in particular, it is problematic to rely on adolescents to communicate with their parents about covering the cost of an IUD in order to receive the protection.
LARC is now the first-line recommended option for contraception among teens. It is time for the province to follow evidence-based practice by removing barriers to LARC and funding it for youth under age 25 across the province.”
Learn more at It is Time to Improve Access to First-Line Contraception for BC’s Youth (2019) by Kelly Anne Cox, MD, MPH Eva Moore, MD, MSPH via BCMJ, 61(4), pp. 178-179 Premise






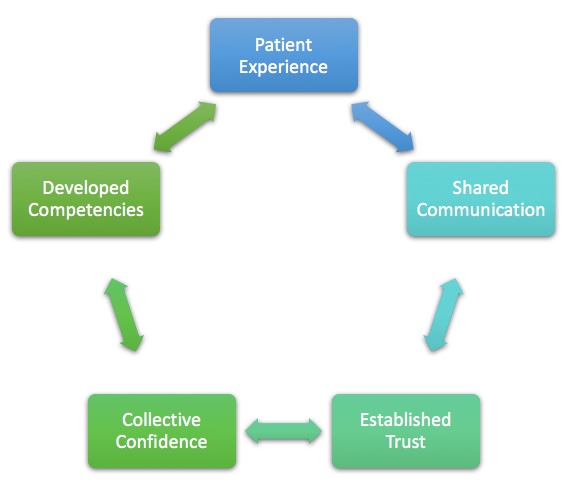 “Confidence is recognized as one of the most influential factors to affect performance. Individual, leader, and team confidence play essential roles in achieving success and the absence of confidence has been connected with failure. While confidence is not a substitute for competency, it creates trusting relationships, empowerment, and resiliency to persevere when challenges arise.
“Confidence is recognized as one of the most influential factors to affect performance. Individual, leader, and team confidence play essential roles in achieving success and the absence of confidence has been connected with failure. While confidence is not a substitute for competency, it creates trusting relationships, empowerment, and resiliency to persevere when challenges arise.