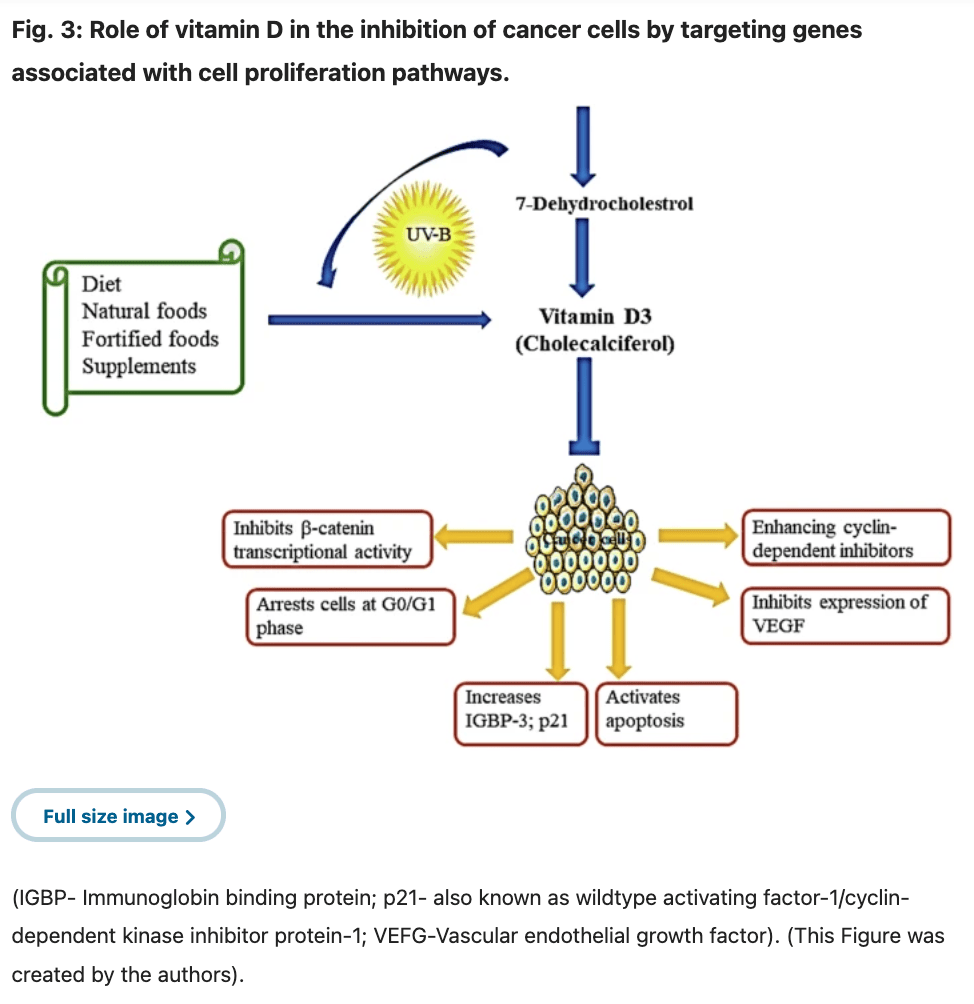
Vitamin D is often associated with bone health, but its role in the body extends much further. It supports immune function, calcium absorption, cellular health, and may play a role in reducing the risk or progression of several non-communicable diseases, including cardiovascular disease, osteoporosis, diabetes, cancer, and thyroid-related conditions.
Despite its importance, vitamin D deficiency remains a widespread global health issue. Many people do not get enough vitamin D through sunlight, diet, or fortified foods. Risk factors include limited sun exposure, darker skin tone, aging, obesity, malabsorption, kidney or liver disease, and low intake of vitamin D-rich foods. Natural sources include fatty fish, cod liver oil, egg yolks, fortified dairy products, fortified plant-based milks, cereals, and UV-exposed mushrooms.
One of the challenges with vitamin D is that recommendations vary across countries and age groups. There is also ongoing debate about the ideal blood level and the appropriate dose for supplementation. Vitamin D status is typically assessed through serum 25(OH)D levels, which help determine whether someone is deficient, insufficient, or sufficient.
Research also shows that absorption is complex. Bioavailability can be influenced by age, digestive health, dietary fat, fibre intake, food processing, disease, and the form of vitamin D consumed. Emerging food technologies, including fortification, microencapsulation, nanoencapsulation, and UV treatment of foods, may help improve vitamin D stability and availability.
The bigger takeaway is that vitamin D deficiency is not just an individual nutrition issue. It is a public health concern linked to broader patterns of chronic disease, diet, environment, access to fortified foods, and health equity. More research is needed to clarify optimal dosing, improve food-based strategies, and understand how vitamin D interacts with genetics, age, sex, geography, and disease risk.
Learn more on Vitamin D: recent advances, associated factors, and its role in combating non-communicable diseases via Nature.