“Human knowledge is never contained in one person. It grows from the relationships we create between each other and the world, and still it is never complete.” ― Paul Kalanithi, When Breath Becomes Air
Recently our Abbotsford-Mission & Chilliwack residents discussed the challenges and opportunities in their transition to practice. The session’s goals were to understand how our program can build on residents’ skills and education as well as provide them the support to explore and determine their path to practitioner. Therefore, we asked participants to identify the resources and vehicles they needed to be successful and then we had them prototype this learning experience.
We initiated the discussion with a live poll to determine how residents currently felt about managing a practice. We then discussed design thinking and its application to medicine. Using this problem-solving method, residents worked in small groups and addressed the following questions:
1. What would help you transition into your role as a practitioner?

Residents indicated that mentorship, business/finance workshops, locum discussions, and hands-on experience in managing a clinic would support their transition to practice as well as provide them the opportunity to ask questions that emerged during their journey. One member recommended that our site create a Practice Management course-pack to be delivered during Academic Half Days. Participants explained that the university and several professional bodies offer courses to assist residents in their transition; however, they described that these classes are in locations that are often inconvenient and offered during times that conflict with their work schedule. Residents also stated that the quality and depth of these sessions vary. One participant suggested that this variance is due to the deficiency in Practice Management curriculum.
2. How would you implement these needs into your educational journey?


Residents identified that their needs would be best met through Practice Management discussions with their preceptors and office staff. Participants also wanted the opportunity to experience running a clinic and suggested designing simulations that would prepare them for an independent practice as well as working their desired schedule. Other ideas included connecting with former graduates to gather pearls of wisdom and increasing our AHD sessions on Practice Management topics.
3. As a group, select one of the ideas and build it as a Resident’s Transition to Practice experience. What would it look like?
Group 1: Simulation Work Week
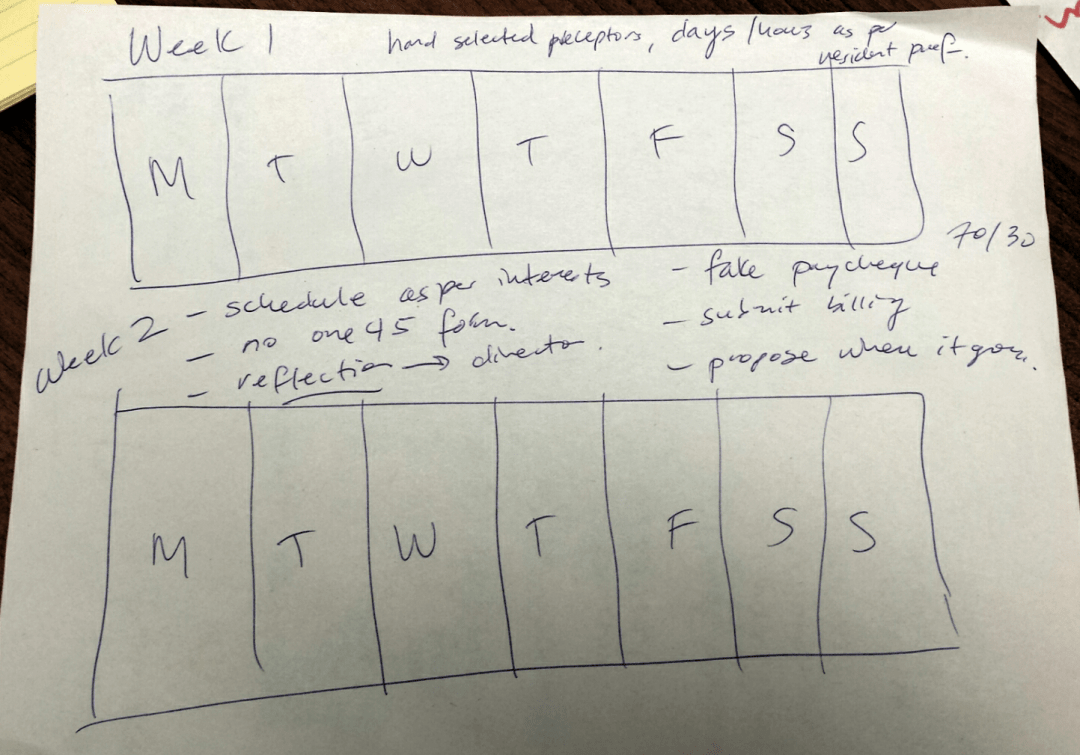
Group 1 designed a 2-week work simulation that allows a resident to experience her/his preferred schedule. The resident would select the primary preceptor; determine the days/hours that she/he projected working; and design the schedule based on her/his interests. During this simulation, the resident would be exposed to topics such as fees and billing. The rotation would be exempt from the program’s formal evaluation process. The simulated experience appeared to be particularly important for those participants who wanted to work in a variety of healthcare settings and/or were parents that needed to understand how their desired schedule impacted their family.
2. Group 2: Preceptor Practice Management Education & Academic Half Day
Group 2 suggested the residency program educate primary preceptors on teaching management strategies to incoming residents. Residents would then have the opportunity to rotate through these clinics and experience their administrative differences. Preceptors would receive a monetary incentive to participate in this module. Group 2 also recommended a series of Academic Half Day sessions focused on understanding and practicing billing codes. Participants discussed creating a pocket billing guide app to help residents and new graduates traverse this increasingly complex terrain.
3. Group 3: Practice Management Academic Half Day Sessions
Group 3 recommended a series of Academic Half Day topics such as day-to-day financial management; locums: negotiating & finding good ones; independent practice; joining a practice; incorporation; logistics & fees; paternity/maternity leave; family planning; CME & Mainpro; and billing. Group 3 also wanted to dedicate time to connecting with former graduates for Q & A. These sessions would be delivered over the final two months of residency. They also described designing a checklist of the “to-do” items prior to graduation.
Once the groups completed their presentations, we then introduced our recent graduate, Dr. Deep Sidhu, who spent the next hour with our residents fielding questions on his experience opening up a new practice.
I want to thank our residents and Dr. Deep Sidhu for their time and input. It’s your honesty that will make this program better and hopefully serve as a model for others to follow. All graduate programs have a responsibility to assist and support their students/residents in their transition to practice. With your continued input, we are aiming to do just that.
Sincerely,
Jacqueline, Program Coach
Additional Resources:
Canadian Medical Association: Practice Management Modules
Doctors of BC: Resource Centre for Residents
University of British Columbia: Transition to Practice
English, D. (2013). Smoothing the transition from resident to attending physician using mentors. Physician Executive Journal.
Holak, E. (2010). Facilitating the transition to practice: A weekend retreat curriculum for business-of-medicine education of United States anesthesiology residents, Journal of Graduate Medical Education, September 2010. J Anesth 24:807–810.
Lister, J. (2010). Evaluation of a transition to practice program for neurosurgery residents: Creating a safe transition from resident to independent practitioner. Journal of Graduate Medical Education.
#designthinking #transitiontopractice #ubcfamilypractice #practicemanagement
