
For more information and registration, click here.

For more information and registration, click here.
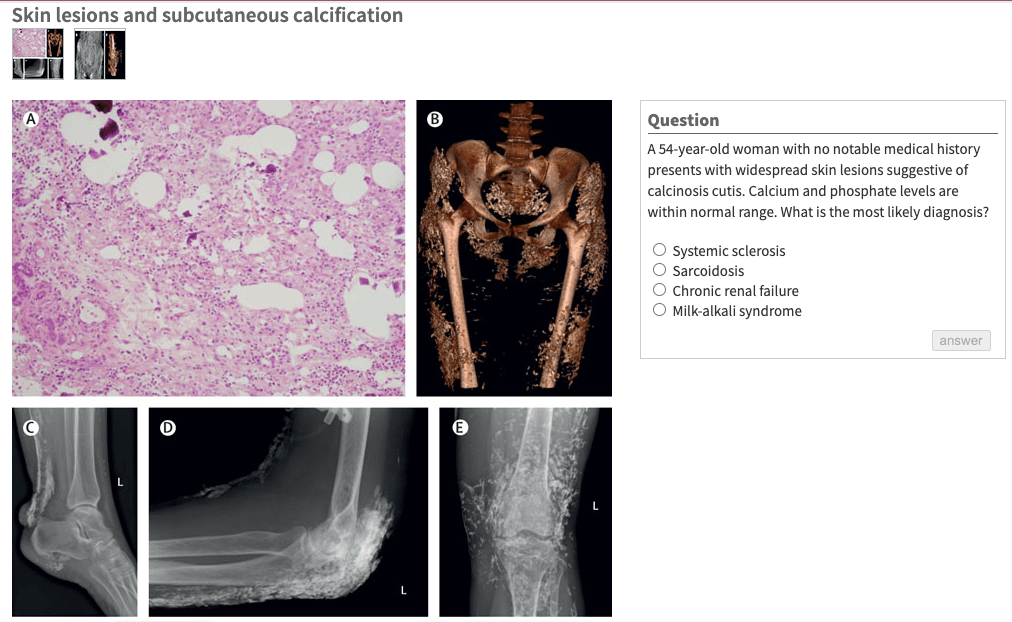
“What is…”
Cue the Jeopardy theme song! Brought to you by Neffy as the winner of the NPR 2021 Tiny Desk Contest.
Click here to answer.
#TheLancet #PictureQuiz
“Our review showed a significant benefit of physical activity interventions of various types on certain outcomes including mobility, ADLs, cognitive function, quality of life and frailty when compared to control groups in frail adults aged 65 years or more. The effect sizes ranged from small to large, with low to moderate certainty of evidence. When we looked at all physical activity interventions together, there was a large effect on frailty, a medium effect on quality of life, ADLs and mobility, and a small effect on cognitive function.
Previous systematic reviews and meta-analyses have been conducted to evaluate various physical activity interventions and their outcomes related to frailty prevention, progression and reversal, but few have used such an explicit inclusion criterion for prefrailty or frailty, or combined individual measurements of outcomes (such as muscle strength and gait speed) into overall effect estimates (such as physical performance) to allow for a more robust presentation of the results. However, frailty itself was measured infrequently, both at baseline and after the intervention. The authors of only 4 of the 23 studies that we meta-analyzed reported frailty outcomes after the intervention, 3 of which were mixed physical activity interventions. When compared to control, these interventions showed a large effect size, with moderate certainty of evidence, similar to other reviews; however, the GRADE approach was not used in any of those reviews, and only 2 included a meta-analysis of outcomes.”
More on the Effectiveness of physical activity interventions in older adults with frailty or prefrailty: a systematic review and meta-analysis via CMAJ.
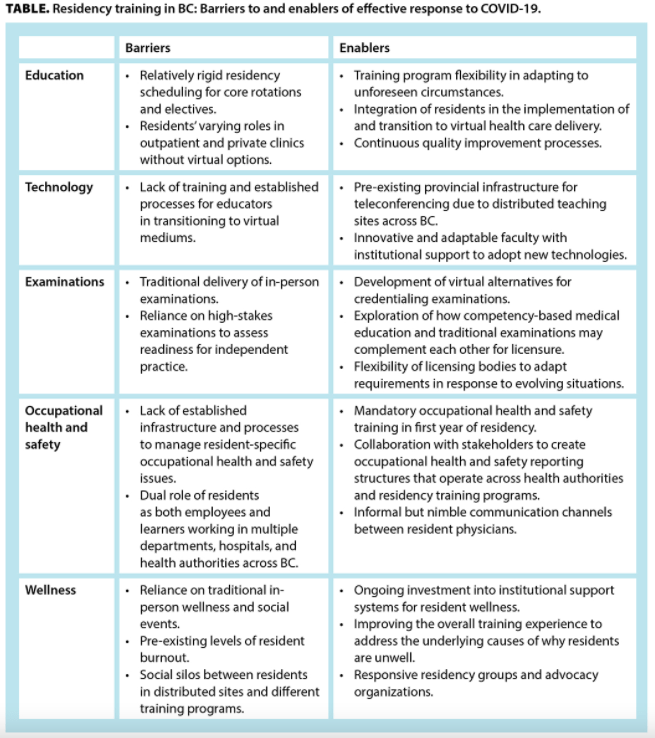
“Residency training programs, hospitals, and Canadian medical education at large recognized these issues, and many positive solutions emerged. The pandemic occurred at a time when many programs were already shifting toward competency-based medical education (CBME), in which training focuses on attaining skill-based milestones rather than traditional time-based requirements. During COVID-19, many training programs embraced the spirit of CBME, espousing flexibility by modifying existing policies to compensate for missed training time because of, for example, redeployment or illness. [10] In addition, many educational opportunities were transitioned to effective virtual formats, as described below. Hence, although many residents experienced the loss of valued learning opportunities, educational adaptations that emerged from the pandemic may continue to benefit future generations of trainees.”
More on Impact of COVID-19 on postgraduate medical education in British Columbia via BCMJ.

“’When something is communicable from person to person, then my having the infection is a risk factor for you,’ he explains. ‘That also means we have the potential for exponential growth. So it’s important that we think about this socially—not just about our individual protection but about how we protect others and also how everyone makes our community a hard target.’” ~ DR. DAVID PATRICK, PROFESSOR, UBC SCHOOL OF POPULATION AND PUBLIC HEALTH
Read more about How to make yourself a hard target for communicable diseases via UBC Beyond.
“Children aged five to 11 in British Columbia had been contracting COVID-19 at higher rates compared with kids in other age groups, but an uptick in vaccination rates has helped reduce those numbers, health officials said Thursday. The province says 550 cases were diagnosed between Oct. 26 and Nov. 1 from 14,295 total cases in that age group since the pandemic began. One of those children went to hospital this week, and between Oct. 26 and Nov., one received critical care, health officials said, as they presented their latest epidemiological modelling during a live news conference.
A total of 56 children aged five and 11 have been admitted to hospital with COVID-19 in B.C. since the pandemic began and four of them required critical care. The province says cases among kids aged nine to 11 rose the most a few weeks after the start of the school year. However, Provincial Health Officer Dr. Bonnie Henry said there have been no hospitalizations in fully vaccinated youth aged 12 to 17 since July.
‘[The vaccine] is working extremely well. We’ve had very few cases and we’ve had no hospitalizations. That’s important for us to think about as vaccines are now becoming available for the younger age group as well,’ she said.”
Read more on COVID-19 cases among kids in B.C. saw highest rise among those 5 to 11 but are declining, health officials say via CBC News.

“It was during the pandemic that I had my first opportunity to meet with a patient approaching end of life. In September 2020, I enrolled in the UBC Legacy Project, where medical students partner with a person who has a life-limiting condition to support them in creating a project to leave with their loved ones. I had been reading about how the coronavirus complicated the grieving process for patients and their families; if there was some way I could help, I wanted to try. So there I was, an inexperienced 22-year-old medical student, donned in PPE, entering a hospice for the first time.”
Read more on Bridging the 6-foot Gap: A medical student’s experience using stories to connect with palliative care patients during the coronavirus pandemic via the BCMJ.

Hello Family Practice Residents,
The Enhanced Skills Global Health program is putting on a series of 4 talks by Dr. Reza Eshaghian. We would like to open up these talks to any Family Practice R1s or R2s who are interested in attending. Please note that these talks are optional and would be additional to any existing academic sessions you have scheduled within your programs.
Global Health Lecture series by Dr. Reza Eshaghian
Dr. Eshaghian is a Clinical Associate at Vancouver General Hospital. He received his MD at University of Western Ontario in 2010 and completed a Rural Family Medicine Residency in Prince Albert Saskatchewan in 2012. After practicing emergency medicine for 4 years, he successfully challenged the CCFP Certificate of Added Competence in Emergency Medicine in 2016. He is licensed in Family Practice with Added Competence in Emergency Medicine with the College of Physicians and Surgeons of BC. He locums in the emergency departments at Richmond and Delta Hospitals and rural communities across British Columbia. Dr. Eshaghian has completed an internship with the World Health Organization (European Office) in 2009, a Diploma in Humanitarian Assistance (Liverpool School of Tropical Medicine) in 2013 and a Diploma in Tropical Medicine and Hygiene with the University of Alabama in 2016. Dr. Eshaghian has worked extensively oversees practicing primary care and emergency medicine in low resource settings. He spends 2 to 5 months yearly (for the last 7 years) with Doctors without Borders / Médecins Sans Frontières. He has been to Ethiopia (twice), South Sudan, Central African Republic, Democratic Republic of Congo, Yemen and recently returned from Syria.
The following article ‘We live in one world‘: Vancouver doctor highlights plight of kids in Syrian detention camps was published recently in The Vancouver Sun regarding his time in Syria.
ALL SESSIONS WILL BE VIA ZOOM Titles and dates of seminar series (all from 7-8:30pm):
October 26: Principles and history of humanitarian relief (Part 1 of 2)
November 4: Structure of humanitarian relief response (Part 2 of 2)
November 8: Severe Acute Malnutrition in low-resource setting
November 10: Infectious Disease in low-resource setting
If you are interested in attending any or all of these sessions, please RSVP.
Lindsay Gowland (She, Her, Hers)
Manager, Enhanced Skills Program
Faculty of Medicine | Department of Family Practice
The University of British Columbia | Musqueam, Squamish & Tsleil-Waututh Traditional Territory
“‘Context matters in medical education’ – is often invoked to defend educational innovation and research that might be seen as lacking transferability and generalisability. Yet context itself and how it works is rarely the subject of research and scholarship. Context does matter; distributed medical education, transnational medical programs and the ongoing disruption to traditional models of clinical placements are all opportunities to advance scholarship that is contextualised to place.
Recent thinking by Bates and colleagues have sought to unpack what context means, using selection and CBME as exemplars of contextualisation. This presentation draws upon critical theories of place from different disciplines to question discourses of deficit and standardisation, explore our recent research findings, and invite discussion on how place and context is experienced in learning and teaching medicine.”
Presenters: Wendy Hu, MBBS, PhD, FRACGP & Tagrid Yassine, MEd, BA, Organisational Learning
Date: Tuesday, November 9, 2021
Time: 12:00pm to 1:30pm PT
For connection details, please email ches.communications@ubc.ca.