
Cue the Jeopardy theme song.
“What is….”
Click here to answer.
#TheLancet #PictureQuiz
“It’s possible to imagine a new organization of doctors that has nothing to do with the business of medicine and everything to do with promoting the health of patients and adroitly confronting the transformational challenges that lie ahead for the medical profession. Such an organization wouldn’t be a trade guild protecting the interests of doctors. It would be a doctors’ organization devoted to patients. Its top priority might be restoring the human factor—the essence of medicine—which has slipped away, taking with it the patient-doctor relationship. It might oppose anti-vaxxers; challenge drug pricing and direct-to-consumer advertisements; denounce predatory, unregulated stem-cell clinics; promote awareness of the health hazards of climate change; and call out the false health claims for products advocated by celebrities such as Gwyneth Paltrow and Mehmet Oz. This partial list provides a sense of how many momentous matters have been left unaddressed by the medical profession as a whole. Tackling any one of them would be hard; perhaps patient-advocacy groups could join in common cause.”
Why Doctors Should Organize: Meeting the challenges of modern medicine will require more than seeing patients (2019) by Eric Topol via The New Yorker.
“Aboriginal people were instrumental in guiding the yarning, helping all participants understand each other, taking time to find the right words to express feelings and discover shared experiences.
The researchers found that many Aboriginal people were happy having non-Aboriginal people involved if they followed ganma and listened. Sometimes it led to a sense of reconciliation between the two groups.
In this context, ganma has come to mean ‘If you listen to us, we’ll listen to you’. That is, two cultures listening to and learning from each other. It’s symbolic, representing different communities working to find practical solutions when dealing with ecological grief and the loss of nature and home.”
More on ‘If the land is sick, you are sick’: An Aboriginal approach to mental health in times of drought: In Australia, psychological tools developed with Aboriginal people can also support farmers whose land is suffering the effects of climate change by Georgina Kenyon via Mosaic.
More on New employment support system coming to Downtown Eastside via CTV News.
More on Trump and Sanders want to ease imports of drugs from Canada. Canada says not so fast by Amanda Coletta via Washington Post.
“An important aspect of Buxton’s work is encouraging the use of respectful, non-stigmatizing language when describing substance use disorders, addiction and people who use drugs. Stigmatization has a direct impact on people who use drugs, she said. It contributes to isolation, which means people who use drugs may use alone and will be less likely to access harm-reduction services or treatment such as a supervised injection site or naloxone, a medication that quickly reverses the effects of an overdose.”
More on UBC researchers help find solutions to the overdose crisis by Thandi Fletcher via UBC News.

 “In any given moment we have two options: to step forward into growth or to step back into safety.”
“In any given moment we have two options: to step forward into growth or to step back into safety.” “Be like water making its way through cracks. Do not be assertive, but adjust to the object, and you shall find a way around or through it. If nothing within you stays rigid, outward things will disclose themselves.” ~ Bruce Lee
“Be like water making its way through cracks. Do not be assertive, but adjust to the object, and you shall find a way around or through it. If nothing within you stays rigid, outward things will disclose themselves.” ~ Bruce Lee
Greetings and hope you are well!
Many of you are just completing your first month of residency and over the past few years some have described the experience to me as drowning, overwhelming, isolating, and stressful. On the whole, these rotations are intensive, brief learning submersions where one is dipped in a culture and way of practice that can often feel foreign and unknown. These “sink or swim” experiences are limited and before a resident can really grasp and acclimate to the learning context they’re moved on to the next rotation.
So, I want to encourage you to check out Martin et al. (2017) Exploring the Experience of Residents During the First Six Months of Family Medicine Residency Training. The article highlights key changes in the transition from medical student to resident and may help in articulating and pinpointing the stress. For example, as one resident from the study explains, “There is an underlying concern that the patient is going to die if I don’t get the diagnosis right.”
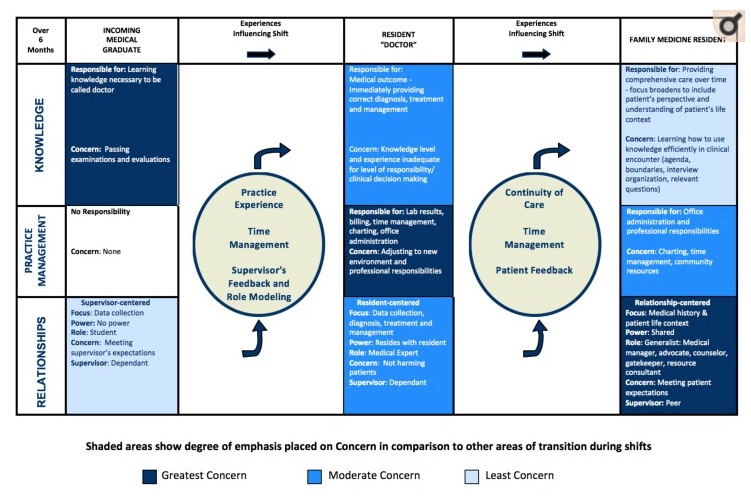
The program’s expectations around knowledge base, practice management, and ability to form and nurture patient relationships have jumped a massive notch. The article offers ideas about acclimating to this new role and building confidence in your environment.
Another read you may want to check out is Flow: The Psychology of Optimal Experience by Mihaly Csikszentmihalyi. I ordered this book for our Preceptors and I believe it currently sits in our Site Library Office so ask Ann for the copy 🙂. I’m particularly fond of this quote:
“Contrary to what we usually believe, moments like these, the best moments in our lives, are not the passive, receptive, relaxing times—although such experiences can also be enjoyable, if we have worked hard to attain them. The best moments usually occur when a person’s body or mind is stretched to its limits in a voluntary effort to accomplish something difficult and worthwhile. Optimal experience is thus something that we make happen. For a child, it could be placing with trembling fingers the last block on a tower she has built, higher than any she has built so far; for a swimmer, it could be trying to beat his own record; for a violinist, mastering an intricate musical passage. For each person there are thousands of opportunities, challenges to expand ourselves.”
~
These rotations, if framed as opportunities, have the potential to expand oneself and to further develop the intrinsic reward system that pushes us past the reluctancy, resistance, and stress of learning something new.
Warmly,
Jacqueline
#WeAreInThisTogether #DesigningTheOptimalExperience #ChangingTheContentsOfConsciousness
Resources:
Martin D, Nasmith L, Takahashi S, Harvey B. Exploring the experience of residents during the first six months of family medicine residency training. Canadian Medical Education Journal 2017; 8(1): 22-36.
Heads up!
MCCQE Part 2 Exam Preparation Course
https://ubccpd.ca/course/mccqe2examprepcourse
Sep 21 (Sat) 0830-1630 | VGH/DHCC | Vancouver BC
Target audience: provisionally licensed IMG physicians
Free, limited spaces!
Up to 6.5 MOC Section 1
Register: https://events.eply.com/mccqe2prep
“Dr. Nadine Caron is the first female Indigenous graduate of the University of British Columbia’s School of Medicine, and the first female Indigenous general surgeon in Canada. Nadine asks us the question, is being the first always good. Recorded at TEDxUNBC in Prince George, BC. Dr. Caron asks us to look at the implications of what it means to be the first person to achieve something.”
Learn more from Dr. Caron on The Other Side of ‘Being First’ via UBC Faculty of Medicine’s Centre for Excellence in Indigenous Health.
#UBCSchoolOfMedicine #DrNadineCaron #TheSilenceOfBeingFirst