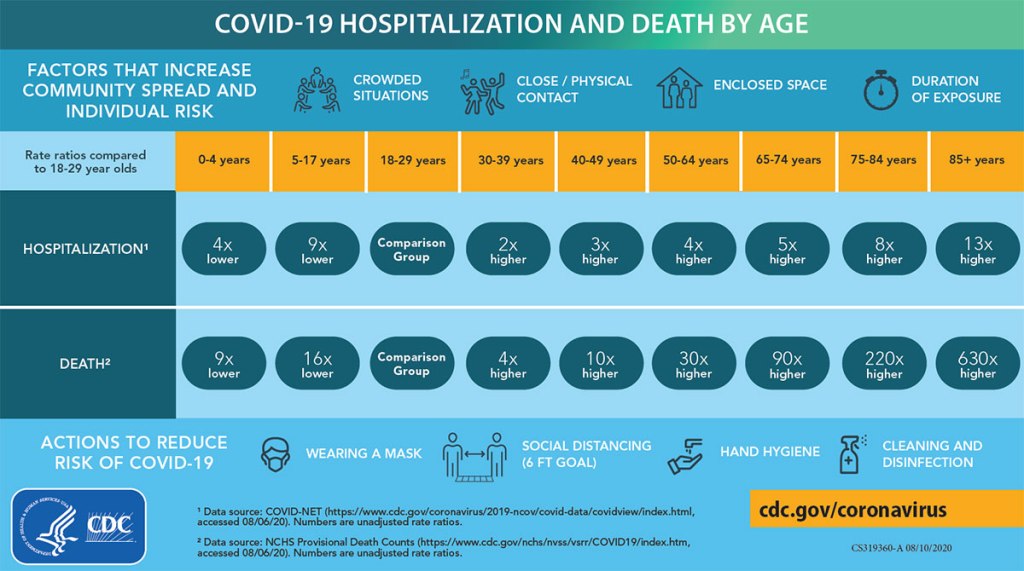
Please take the proper precautions and actions to reduce the risk of COVID-19.
More information here at the CDC National Center for Health Statistics.

Please take the proper precautions and actions to reduce the risk of COVID-19.
More information here at the CDC National Center for Health Statistics.
Women’s Health Research Cluster (WHRC) hosts a virtual conference series on Women’s Brain Health
From September 2020 – June 2021 the WHRC will bring you monthly events featuring world renowned speakers to discuss and share information about a variety of brain health issues that women face. Come connect with like-minded peers at one of our workshops, symposia, networking sessions or trainee/mentor events.
You can register for the full series, or pick and choose which event you want to go to. Full series registration grants you access to all post-event recordings. Click here to learn more.
To create more awareness and better prepare early-career physicians to care for LGBTQ+ patients, a team from the University of Toronto have developed a new LGBTQ+ health workshop for resident physicians.

Drs. Tehmina Ahmad, Michael Scott and Jacqueline James, a professor with the Department of Medicine, alongside Wilson Center Researcher Miranda Schreiber, developed this workshop as a way of calling attention to the unique needs and health disparities faced by LGBTQ+ people.
The workshop supports the following objectives:
If you are interested to learn more, please contact Miranda Schreiber at miranda.schreiber@mail.utoronto.ca or visit here.
Simulation cases available on Airway, Infections, Pediatric, Rural, Trauma, Shock, Respiratory, and more via BC Emergency Medicine Network and BC Simulation Network.
Thank you Dr. Wojtera for sharing!
The Office of Faculty Development and the Centre for Health Education Scholarship are pleased to co-facilitate the CAME Webinar Series at UBC. Designed to bring practical, evidence and experience-based advice to Canadian health educators, the webinars offer the opportunity to engage online with an expert and with colleagues in a live discussion on a key topic in health professions education.
*Please note that while these sessions are free to attend, registration is required. See registration link below.
Bias and the Educator: Exploring Implicit, Explicit, and Structural Bias in Medical Education
Presenter: Dr. Javeed Sukhera, Western University
Date: Tuesday, October 20, 2020
Time: 9:00 to 10:00 am
Register here.
“Children are widely recognized as a vulnerable population during disasters and emergencies. In BC there are growing concerns that children may be at higher risk of abuse and neglect as a consequence of the current COVID-19 pandemic and the public health measures to limit its spread. Increased family and financial stress, disrupted routines, and lack of access to community supports can all contribute to child maltreatment. At the same time, physical distancing has restricted contact between children and the protective adults, such as teachers, who most commonly report cases of suspected child maltreatment. Despite the pandemic, physicians continue to interact with children and families and are uniquely situated to identify cases of suspected child maltreatment. All physicians have a role to play in ensuring the safety and protection of children. Specific approaches to clinical practice in the pandemic era and resources adapted for the pandemic can help physicians assess risk of child maltreatment, support children and families, and recognize and respond to child abuse and neglect.”
Learn more on Child Abuse and Neglect in the COVID-19 Era: A Primer for Front-Line Physicians in British Columbia by Kristopher T. Kang, MD & Nita Jain, MD, FRCPC via BCMJ.

The World Health Organization has stated that the climate crisis is the biggest health concern of the 21st century–and the Lancet has said that fighting climate change could be the greatest global health opportunity. If we do not make major changes to reduce greenhouse gas emissions in the next 10 years, the Intergovernmental Panel on Climate Change (IPCC) predicts catastrophic effects on the environment and human health. This conference will inspire us all in our health care roles to better understand these issues and advocate for necessary systemic change.
Register here for the October 30, 2020 event.
I also want to encourage you to check out the Virtual Showcase which is accepting submissions until September 25.

Register at www.whri.org.

“Students, staff, and visitors at UBC will be required to wear non-medical masks when indoors on campus as of Wednesday, September 16.
The school’s previous policy ‘strongly recommended’ the use of masks.
‘UBC is implementing a new measure to help limit COVID-19,’ Santa J. Ono, president and vice-chancellor, says in a release.
‘The health and safety of the UBC community is our first priority, and we continue to monitor COVID-19 and follow effective safety practices as understanding of the virus evolves. The requirement to wear non-medical masks indoors recognizes that transmission is reduced when face masks are worn in conjunction with physical distancing and other safety practices.'”
Read more here.
#UBC #WearAMask
“Most scientists and health authorities support wearing non-medical face masks in public to help prevent the spread of COVID-19. A team of UBC researchers led by Steven Rogak, a professor of mechanical engineering who studies aerosols, and Dr. Jane Wang, a clinical instructor in the faculty of medicine, decided to test the most popular types of mask fabrics to find out how well they filtered particles while remaining breathable.
How do DIY masks stack up against commercial non-medical masks?
Rogak: Our results showed that a mask with two layers of low-thread-count quilting cotton is both comfortable and breathable. In fact, such a mask with an added three-ply dried baby wipe filter was as effective as a commercial non-surgical mask at stopping particles, and almost as breathable. It filtered out up to 80 per cent of 3-micron particles, and more than 90 per cent of 10-micron particles.
Wang: The COVID-19 particle is only around 0.1 micron in size, but it is always attached to something larger, like the droplets produced by breathing, talking and coughing, which are typically larger than 5 microns. An N95 mask can filter most particles 0.3 microns or larger, but even an N95 mask is going to take in large, massive droplets with lots of viruses if it does not seal against the face. A well-fitted, well-designed cloth mask with a baby-wipe filter will be more effective at filtering 5- or 10-micron particles than a poorly fitted N95 mask.”
Learn more about their findings here on UBC researchers run tests to find best materials and styles for face masks via UBC News.