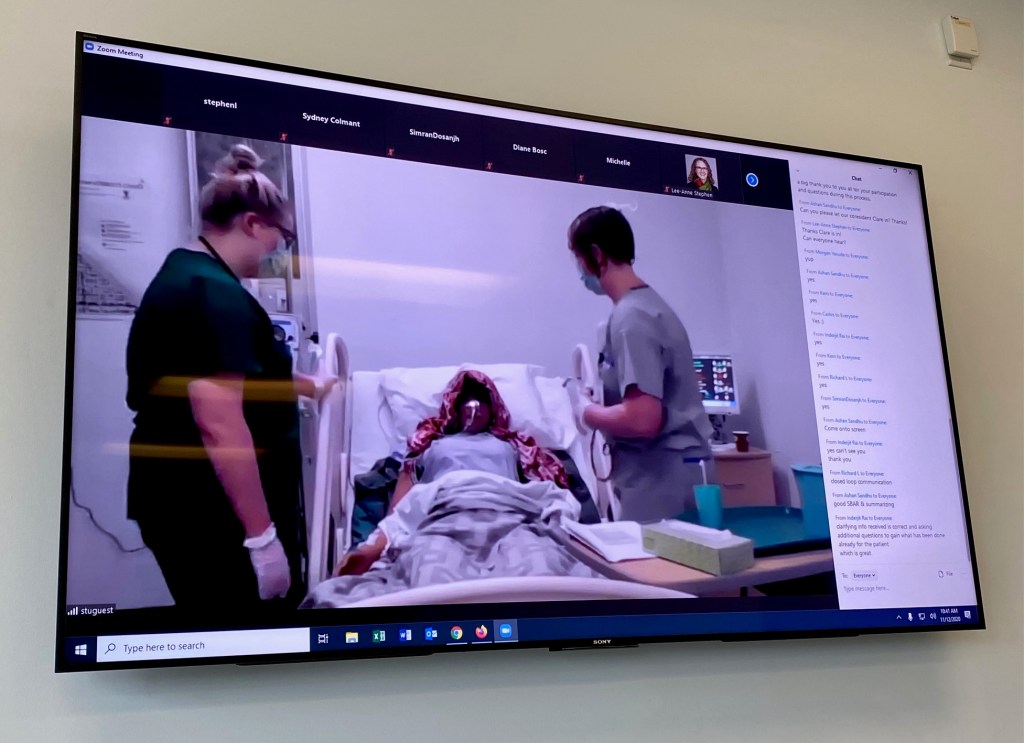
This past week we conducted our first University of the Fraser Valley (UFV) and University of British Columbia (UBC) interprofessional virtual simulation. Our UFV-UBC faculty have worked over the past year to design this unique opportunity that bridges Nursing and Family Practice programs in order to support team-based communication and patient-centred care. During the course of three hours, we facilitated four simulations that involved two teams comprised of one nursing student and one resident. Each team participated in two simulations that addressed caring for a critically ill patient followed by breaking bad news to the patient’s caregiver. Our learning objectives focused on:
- Demonstrating effective, collaborative, and respectful interprofessional communication
- Developing knowledge of health care team members roles
- Demonstrating collaborative leadership skills when caring for a critically ill patient
- Managing the care of a deteriorating/changing patient
We want to thank our simulation participants including Claire Wilcox, Megan Schmidt, Dr. Sophia Park, and Dr. Casey Hicks, in addition to our learners that joined us from home. We would also like to acknowledge the UFV-UBC faculty that were instrumental in developing and facilitating the simulation including Lee-Anne Stephen, Sarah Johanson, Janelle Baerg, Dr. Thanh Luu, and Dr. Jacqueline Ashby. Lastly, we thank UFV for allowing our team to use their facilities.
I want to conclude by saying that COVID-19 has challenged our program’s ability to both protect our learners’ health and offer them the experiences that are instrumental in their growth and development as healthcare practitioners. As a community, it’s imperative that we all do our part in taking the necessary measures to stop the spread of this virus. Please review the new regional orders that pertain to social gatherings, travel, indoor group physical activities, and workplace safety.
We are in this together.
Thank you,
Jacqueline